Recent manuscripts
Archive
Editorial Board
Aims and Scope
Open Access
Indexing
Contact us
Authorship & COI
Principles of Transparency Checklist
Publication Ethics
Crossmark
Data Policies
Supporting Diversity
Instructions to authors (PDF)
Manuscript Types
Manuscript Formatting
How to submit
Special Publications & Reprints
Preprints
The impact of nicotine metabolite ratio on pharmacotherapy effectiveness in real-world settings: a longitudinal analysis
1
University College London, United Kingdom
2
University of Stirling, United Kingdom
3
King’s College London, United Kingdom
4
University of Toronto, Canada
Publication date: 2018-03-01
Tob. Induc. Dis. 2018;16(Suppl 1):A518
KEYWORDS
TOPICS
ABSTRACT
Background:
Future developments in tobacco control are likely to involve personalisation of treatment to improve efficiency. Pharmacotherapy provision based on Nicotine Metabolite Ratio (NMR) status has been shown to improve outcomes in clinical trials: normal relative to slow metabolisers benefit more from varenicline than nicotine replacement therapy (NRT) treatment. However, it is unknown whether this effect translates to other settings.
Methods:
Data come from 1,563 participants attending English Stop Smoking Services in 2012/13. Sociodemographic, mental/physical health, smoking (dependence, determination to quit) and treatment characteristics (varenicline vs. NRT; group vs. one-to-one behavioural support) were assessed at baseline. Baseline salivary nicotine metabolites were measured and NMR (3-hydroxycotinine/cotinine) status computed, characterising smokers as slow (NMR< 0.31, N=454) or normal (NMR≥0.31, N=1,109) metabolisers. Carbon-monoxide verified 2-week and 50-week continuous abstinence was assessed at 4-week and 52-week follow-up post-quit, respectively. The association between abstinence rates and predictor variables was determined using log-binomial generalised linear models that included a pharmacotherapy by NMR status interaction term and controlled for all covariates. All analyses were intention-to-treat.
Results:
Of participants, 44.2% (95% confidence interval (CI) 41.8-46.7%) and 8.0% (95%CI 6.8-9.5%) were continuously abstinent at 4-week and 52-week follow-up, respectively. There was no evidence of a pharmacotherapy by NMR status interaction on either outcome in adjusted analysis (see Figure). Higher abstinence rates were independently associated with higher socio-economic group, treatment with varenicline, lower dependence and greater age at both follow-ups and with greater determination to quit and group support at 4-week follow-up, only.
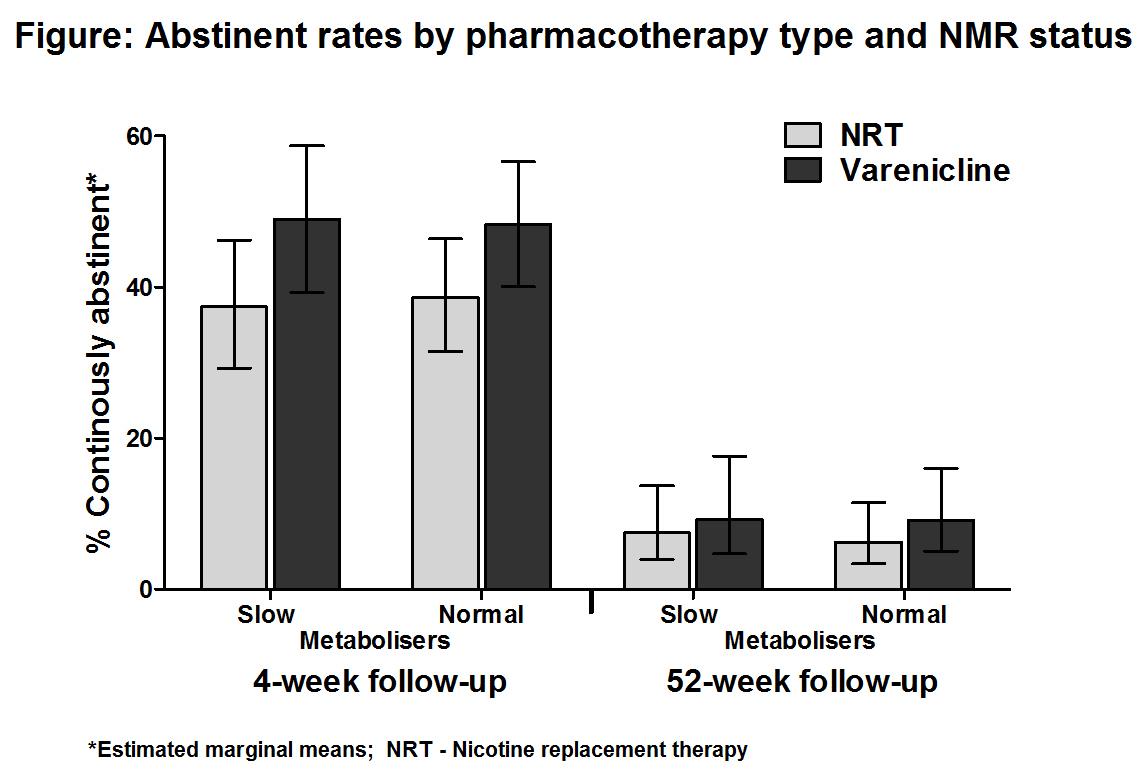
[Figure]
Conclusions:
Our study did not replicate clinical trial data, indicating that NMR status does not substantially contribute to differential pharmacotherapy effectiveness in Stop Smoking Services. As this was an observational study, self-selection or unmeasured confounders may have influenced results. However, this suggests the effect of NMR in real-world settings is likely to be small, context-dependent and therefore may not translate globally.
Future developments in tobacco control are likely to involve personalisation of treatment to improve efficiency. Pharmacotherapy provision based on Nicotine Metabolite Ratio (NMR) status has been shown to improve outcomes in clinical trials: normal relative to slow metabolisers benefit more from varenicline than nicotine replacement therapy (NRT) treatment. However, it is unknown whether this effect translates to other settings.
Methods:
Data come from 1,563 participants attending English Stop Smoking Services in 2012/13. Sociodemographic, mental/physical health, smoking (dependence, determination to quit) and treatment characteristics (varenicline vs. NRT; group vs. one-to-one behavioural support) were assessed at baseline. Baseline salivary nicotine metabolites were measured and NMR (3-hydroxycotinine/cotinine) status computed, characterising smokers as slow (NMR< 0.31, N=454) or normal (NMR≥0.31, N=1,109) metabolisers. Carbon-monoxide verified 2-week and 50-week continuous abstinence was assessed at 4-week and 52-week follow-up post-quit, respectively. The association between abstinence rates and predictor variables was determined using log-binomial generalised linear models that included a pharmacotherapy by NMR status interaction term and controlled for all covariates. All analyses were intention-to-treat.
Results:
Of participants, 44.2% (95% confidence interval (CI) 41.8-46.7%) and 8.0% (95%CI 6.8-9.5%) were continuously abstinent at 4-week and 52-week follow-up, respectively. There was no evidence of a pharmacotherapy by NMR status interaction on either outcome in adjusted analysis (see Figure). Higher abstinence rates were independently associated with higher socio-economic group, treatment with varenicline, lower dependence and greater age at both follow-ups and with greater determination to quit and group support at 4-week follow-up, only.

[Figure]
Conclusions:
Our study did not replicate clinical trial data, indicating that NMR status does not substantially contribute to differential pharmacotherapy effectiveness in Stop Smoking Services. As this was an observational study, self-selection or unmeasured confounders may have influenced results. However, this suggests the effect of NMR in real-world settings is likely to be small, context-dependent and therefore may not translate globally.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.

